Petechiae: Causes, Treatment & When to See a Doctor
Petechiae are tiny red spots, usually less than 2 mm, that form on the skin and membranes lining body surfaces like the mouth and eyes. The non-blanching rashes have multiple causes, making them common among different age groups. While most cases are mild, you might need to see a doctor promptly as petechiae can be a sign of a serious underlying medical problem.
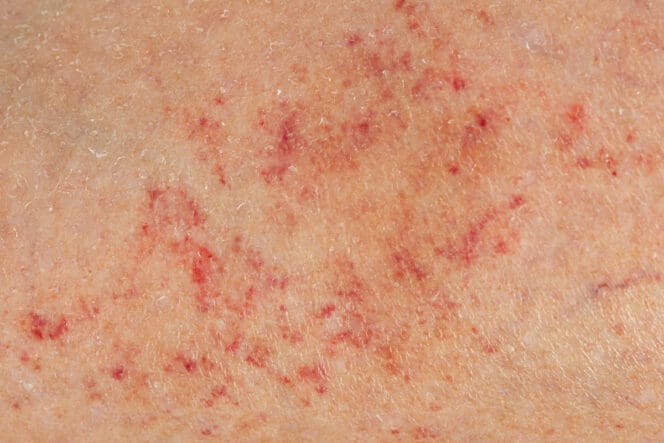
What Are Petechiae?
Petechiae are pinpoint-sized spots that appear on the skin and mucous membranes because of bleeding from the capillaries below these surfaces. They can appear as red, brown or purple lesions that do not disappear when squeezed. Because of that, petechiae are described as non-blanching.
When tiny blood vessels (capillaries) break, the bleeding into the skin results in multiple small spots called petechiae.
Typical petechiae occur in clusters, resembling a rash. However, they are neither bumpy nor itchy like most rashes. When you press a distinctive rash, it becomes lighter or pale. But petechia retains its characteristics even after pressing.
Petechiae are usually less than 2 mm and any spot of bleeding greater than 2 mm is classified differently because of the distinct causes. Petechial lesions can occur anywhere on the body irrespective of age, but the children are most affected.
What Causes Petechiae?
When tiny blood vessels (capillaries) break, the bleeding into the skin results in multiple small spots called petechiae. Different conditions, ranging from mild, preventable diseases, life-threatening illnesses, and prescription drugs, can cause this bleeding below the skin or mucous membranes.
Here are the conditions that might be responsible for your skin lesions:
| Condition | Description | Other Symptoms |
| Invasive Meningococcal Disease | A life-threatening disease of the central nervous system caused by the bacteria Neisseria meningitides. It is common in children. | Headache, neck pain, fever, light sensitivity, and vomiting |
| Endocarditis | Inflammation of the inner heart layer, including the valves | Shortness of breath, fever and chills, fatigue, and generalized body aches |
| Leukemia | Cancer of the blood cells and bone marrow | Unintended weight loss, easy bruising with bleeding from gums and nose, fever, and night sweats |
| Thrombocytopenia | Low platelet counts resulting from either autoimmune reactions or reduced production | Bleeding gums, nose bleeding, blood in urine or stool, and yellow eyes or skin |
| Mononucleosis | A viral infection, also known as mono or kissing disease, is most prevalent among young adults/teens. | Sore throat, fever, swollen tonsillar glands, muscle pain, fatigue |
| Vasculitis | A disorder affecting the blood vessels with inflammation followed by thickening of the vessel wall | Fatigue, fever, headache, peripheral neuropathy (numbness and weakness), or even stroke |
| Viral Hemorrhagic Fevers | Diseases like Ebola, Marburg, and Dengue that disrupt blood clotting mechanisms | Generalized body weakness and pain, high fever, as well as bleeding from body orifices |
| Other Infections | Other common bacterial and viral diseases such as Rocky Mountain Spotted Fever and Hantavirus | Fever, general body weakness, aches, sore throat, swelling glands, nausea, and vomiting |
| Scurvy | Inadequate vitamin C in the body | Painful joints, gum swelling, easy bruising, and breathlessness |
| Prolonged Straining | Activities like weightlifting, vomiting, giving birth, or coughing can cause petechial hemorrhages. | |
| Medications | Antibiotics like penicillin, anticonvulsants including phenytoin and some antidepressants |
Diagnosis
The investigations for the diagnosis of petechiae are as varied as the causes themselves. First, your doctor will take a comprehensive medical history to identify the possible risk factors and other associated symptoms that point to particular aetiologies. A thorough physical examination helps to localize the lesions and rule out other indicators of life-threatening illness by checking the ears, throat, lungs, and heart.
Some of the parameters your doctor will measure include blood pressure, heart rate, temperature, and joint motion. Tests such as urinalysis, renal and liver function tests, coagulation profile, complete blood count, and bone marrow biopsy can indicate the cause of the bleeding. Markers of inflammation like CRP and procalcitonin can also be useful.
If the trigger for the petechiae is obvious, for instance, in the case of prolonged straining, complex procedures such as bone marrow biopsy are not necessary.
Treatment Options
If you or your child have petechiae that spread quickly, or if you have dots plus other symptoms, seek medical attention.
Cleveland Clinic
Like the causes of petechiae, the treatment options vary, ranging from lifestyle changes, medical prescriptions to surgery. For petechiae caused by trauma or straining, the treatment can be as simple as bed rest. However, it is essential to seek professional help before starting treatment due to potential complications of poorly managed petechial hemorrhage.
Home Remedies for Petechiae
In most cases, petechiae will not require any specific treatment. If your doctor recommends monitoring of the lesions without prescribing any medications, it is likely that your condition is mild and will resolve on its own.
Here are home remedies that you can use in restoring your skin appearance:
- Cold compresses
- Rest with extra fluid intake
- Over-the-counter medications like NSAIDs
- Switching to lighter weights if your petechiae are due to weightlifting
Diet modification is crucial in dealing with petechiae, primarily caused by vitamin K or vitamin C deficiency. Eating foods rich in these vitamins, such as dark green leafy vegetables for vitamin K, can help with healing the tiny spots.
If medications are responsible for your petechiae, discontinuing the associated drug and seeking an alternative is recommended. The drugs that can cause petechiae include phenytoin, quinine, and penicillin.
Specific Treatment
Following investigations, your doctor might identify a specific cause of the petechiae and recommend the appropriate therapy, which can be:
- Antibiotics against bacterial infections such as meningococcal disease
- Anticancer drugs or radiation therapy to treat leukemia
- Corticosteroids to reduce inflammation of the blood vessels
- Surgery, either bone marrow transplantation or splenectomy to reverse thrombocytopenia
- Immune-suppressing drugs to treat autoimmune conditions like SLE
- Vitamin K or C supplements
Possible Complications
While the petechial lesions usually heal without scarring, the underlying conditions can result in complications if not treated appropriately. Potential complications include:
- Kidney damage from diseases such as Henoch-schnolein purpura and SLE
- Bleeding in the brain associated with bleeding disorders such as thrombocytopenia
- Sepsis resulting from the spread of bacterial infections to different organs. Sepsis can also cause end-organ damage, especially to the kidney and liver.
- Heart disease
Prevention
Prevention of petechiae requires you to understand the possible causes and avoid them. However, not all the underlying conditions are preventable.
If certain drugs give you petechial marks, you need to avoid these medicines. Every time you visit a doctor, you should inform them about such medications so that they provide alternatives and prevent recurrence of symptoms.
Some organisms that cause infections leading to petechiae can be transmitted from one person to another. To prevent such conditions, you should:
- Avoid using items that have touched someone else’s mouth without washing.
- Observe proper hand hygiene by regularly washing your hands with soap and water or rubbing with an alcohol-based sanitizer.
- Avoid close interaction with individuals who appear sick, as some viral causes of petechiae are contagious.
- Clean counter-tops and other high-touch surfaces like door handles regularly.
- Apply DEET-containing insect repellants before going into woody or grassy areas to prevent tick bites. Wearing long-sleeved shirts and pants when entering grasslands will also offer additional protection.
When Should I See a doctor?
Petechiae can indicate a severe underlying disease, especially in young children. You should contact a doctor when you or your child develops non-blanching red spots of less than 2 mm with any of the following associated symptoms:
- Altered mental status, including confusion and loss of consciousness
- High fever
- Shortness of breath
- Rapidly spreading petechiae
- Petechiae without any apparent cause like trauma
FAQs
What is the main cause of petechiae?
Infections by bacteria and viruses remain the leading cause of petechiae among different age groups. In children with petechiae and high fever, invasive meningococcal disease is considered the first diagnosis. Drug reactions are also implicated in a substantial number of cases.
Should I worry about petechiae?
You do not need to worry about these lesions in most instances unless they co-occur with fever, spread rapidly, or are associated with shortness of breath.
Is petechia life-threatening?
On their own, petechiae are not life-threatening. However, some underlying conditions such as invasive meningococcal disease are regarded as medical emergencies requiring immediate attention.
What deficiencies cause petechiae?
Vitamin deficiencies such as vitamin C and K are major causes of petechiae. A diet rich in vitamin K such as green leafy vegetables and vitamin C supplements can help prevent petechial hemorrhages.
References
-
Petechiae. (September 2021). NCBI.
-
Clinical Practice Guidelines-Petechiae and Purpura. (February 2021). The Royal Children’s Hospital Melbourne.
-
Purpuric and petechial rashes in adults and children: initial assessment. (March 2016). The BMJ.
-
American Society of Hematology 2019 guidelines for immune thrombocytopenia. (December 2019). American Society of Hematology.
-
Petechiae. (June, 2021). Cleveland Clinic.
-
Fever With Petechiae In An Infant: Diagnostic And Treatment Conundrum. (January 2018). Society of Critical Care Medicine.
Last Updated February 26, 2022
Note: This page should not serve as a substitute for professional medical advice from a doctor or specialist. Please review our about page for more information.