Ocular Rosacea: Symptoms, Causes & Treatment
Ocular rosacea is a chronic inflammatory disease affecting the eyes and skin around the eyes. It is a form of rosacea, a chronic skin disease that causes the face to appear flushed.
Approximately 5 percent of people worldwide have some form of rosacea. It affects more than 14 million Americans and 415 million people around the world.
Rosacea commonly affects the cheeks, nose, forehead, and chin. In some patients, the eyes are not affected, and in others, only the eyes are affected.
Recent research confirms that more than 50 percent of rosacea patients show symptoms in the eyes. Ocular rosacea is often overlooked as dry eyes, irritated eyes, seasonal allergies, or problems with contacts.
Currently, there is no known cause or cure for ocular rosacea. Research studies link rosacea flare-ups to specific environmental factors, certain foods, and stress.
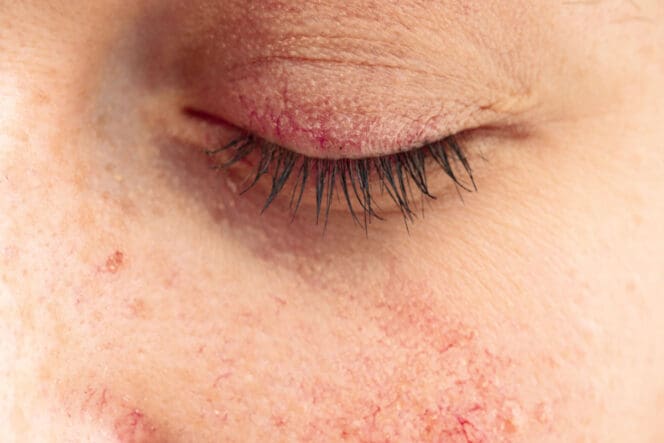
Ocular Rosacea Symptoms
Symptoms of ocular rosacea typically include the following:
- Eye dryness
- Light sensitivity
- Stinging sensations
- Swelling around the eyes
- Bloodshot eyes
- Crusty discharge in the eyelashes
- Recurring styes
Symptoms may appear as other complications, such as dry eye or blepharitis, and swollen or inflamed eyelids.
A recent study from the Journal of the American Academy of Dermatology showed that about 20 percent of patients experience ocular findings before showing rosacea on the skin.
Vision may be blurry. It may feel as if there is a foreign body in the eye. In addition, there may be external signs along the lid margin.
Severe cases of ocular rosacea can lead to corneal inflammation and scarring. This can result in corneal perforation and vision loss.
Causes of Ocular Rosacea
Research studies are investigating the causes of rosacea along several lines:
- Genetics: The condition may be inherited and run in families.
- Inflammation: Blood vessel swelling may result in redness and flushing.
- Mites: They can clog the glands in the face, leading to swelling and irritation.
- Bacteria: There may be a link to Helicobacter pylori bacteria, which is also found in gastrointestinal diseases.
As researchers continue to investigate the origins for this condition, studies are ongoing to understand triggers that may cause flare-ups. Typically, the triggers are related to environment, diet, and stress.
Risk Factors for Rosacea
Rosacea is known for flare-ups and remissions. For this reason, individuals need to understand personal risk factors. These may include environmental and lifestyle factors that help individuals achieve and maintain remission.
Ocular rosacea is more likely to develop in people who meet the following criteria:
- Between 30 and 50 years old
- Women
- People with light skin
- Western European ethnic background, especially from England and Scotland
While this condition is often found in individuals with fair skin, it can also occur in people with dark skin.
Diagnosis
To diagnose ocular rosacea, your doctor or health care provider will perform a physical exam, take your medical history, and evaluate your symptoms.
There are no dedicated tests to diagnose ocular rosacea. The diagnosis will rely on the physical exam as well as your answers to questions.
See your doctor as soon as you notice symptoms to get an early diagnosis and start treatment. Early intervention can prevent the condition from worsening.
Treatment for Ocular Rosacea
Treatment approaches for ocular rosacea include prescription medication, over-the-counter options, home remedies, and lifestyle changes.
Medical Treatment
Eyelash hygiene is essential to keep the eye clean and calm. Your doctor may recommend a variety of medical approaches to reduce flare-ups.
Oral omega-3 supplements and eyelash hygiene are often recommended together. These are often followed by gently applying azithromycin and calcineurin inhibitors to the skin.
Recent studies confirm that it is possible to control this disease with therapeutic modalities, such as topical corticosteroids, topical cyclosporine, and systemic doxycycline. Azithromycin applied topically may be as effective with fewer adverse effects than oral doses of doxycycline.
Steroid eye drops and ointments may be prescribed to reduce redness and swelling, while antibiotic pills or ointments may be prescribed to treat any infection.
Artificial tears or lubricating eye drops may be used to keep eyes moist. Eye drops to reduce redness can irritate the eyes and make symptoms worse, so avoid these.
Rosacea on the face is often reduced or controlled with a blend of therapies, including topical medications, oral therapies, and light devices.
Home Remedies
Rosacea is a chronic condition. While it may not be curable, it can be managed.
- Eyelid hygiene: Ocular rosacea starts at the eyelid, making good eyelid hygiene a top priority. Cleanse the eyelashes twice daily with a special eyelid wash or gentle baby shampoo, applied to a wet, clean washcloth. A warm compress may be helpful on closed eyelids.
- Supplements and holistic approaches: Omega-3 with GLA fatty acid found in evening primrose or bilberry is sometimes recommended for ocular rosacea. Turmeric may be useful in reducing inflammation. Tea tree oil is another option used to counteract inflammation.
Flare-Up Prevention
Lifestyle modifications aim to reduce flare-ups by minimizing contact with triggers. As a result, prevention is closely linked with understanding your personal triggers. Flare-ups have been connected with stress, diet, and seasonal changes.
Making overall lifestyle changes can help to reduce rosacea flare-ups, reducing their frequency and severity. These changes may include diet modifications, such as avoiding foods that dilate blood vessels like caffeine, alcohol, and spicy foods.
Certain activities, environments, and foods affect individuals differently and may trigger flare-ups for some people and not others. To prevent flare-ups, it is essential to track what things seem to trigger your flare-ups.
Potential triggers can be separated into different categories:
- Environmental: Triggers may involve being outside in sunny, windy, hot, or cold conditions. Pay attention to the weather and how it affects your rosacea.
- Sports: Being very physically active, such as running, biking, or hiking, can trigger a flare-up for some.
- Exposure to UV light: This may include natural sunlight or artificial UV light like tanning beds.
- Food and drink: Certain foods and drinks may trigger rosacea flare-ups, such as alcohol, hot coffee or tea, spicy food, or other specific ingredients.
- Stress: Physical or emotional stress can trigger a flare-up. Engage in activities that promote relaxation like yoga or meditation.
The more you can manage your triggers, the better you can control your ocular rosacea. If you aren’t sure where to start, contact your health care provider to create a plan together.
Ocular Rosacea FAQs
What is the best treatment for ocular rosacea?
The best treatment for ocular rosacea is quite individualized. Understand your triggers, and develop a treatment plan with your health care provider. If you follow the treatment plan as best as you can, it will minimize the impact of ocular rosacea in your life.
What causes ocular rosacea flare-ups?
Different people have different triggers that ignite flare-ups. To reduce your flare-ups, consider your lifestyle, habits, nutrition, and exposure to environmental factors. Evaluate how to limit sun exposure, get enough quality sleep, monitor your diet, and find ways to cope effectively with stress.
Does ocular rosacea go away?
Ocular rosacea does not go away, but it can be managed. With proper management, it can have less of an impact on your daily life.
This is a chronic condition that can be managed with eyelid hygiene, a personalized treatment plan, and lifestyle modifications. It might take a few days or weeks for steroid eye drops or other medications to start working. Your progress will depend on the severity of your flare-ups, your triggers, and your treatment regime.
Is ocular rosacea an autoimmune disease?
While rosacea has been linked to certain autoimmune disorders, no one knows exactly what causes the condition. It has not been proven that it is caused by an autoimmune condition.
References
-
Ocular Rosacea. American Academy of Ophthalmology.
-
Rosacea: Who Gets and Causes. American Academy of Dermatology Association.
-
Rosacea Treatment: Eye Problems. American Academy of Dermatology Association.
-
Ocular Rosacea: Symptoms, Causes & Treatment. Cleveland Clinic.
-
Ocular Rosacea: Common and Commonly Missed. (April 2013). Journal of the American Academy of Dermatology.
-
Ocular Rosacea: What Your Eyes May Be Trying to Tell You. National Rosacea Society.
-
Genetic Disorders. Cleveland Clinic.
-
Researchers Make Advances in Understanding Ocular Rosacea. National Rosacea Society.
-
Gastrointestinal Diseases. Cleveland Clinic.
-
Understanding the Origins of Ocular Rosacea. John Hopkins Medicine.
-
Rosacea Symptoms & Treatments. National Health Service (NHS).
-
Clinical Findings, Follow-Up and Treatment Results in Patients With Ocular Rosacea. (January 2016). Turkish Journal of Ophthalmology.
-
ODs Can Help Patients Control Rosacea Symptoms. (April 2019). Primary Care Optometry News.
-
Eye Drops. American Academy of Ophthalmology.
-
Lubricating Eye Drops for Dry Eyes. American Academy of Ophthalmology.
-
Rosacea. John Hopkins Medicine.
-
Ocular Rosacea. (November 2020). Current Opinion in Ophthalmology.
-
Therapeutical Management for Ocular Rosacea. (January–April 2016). Case Reports in Ophthalmology.
-
Topical Azythromicin in the Treatment of Ocular Rosacea. (April 2011). Investigative Ophthalmology & Visual Science.
-
Researchers Make Advances In Understanding Of Ocular Rosacea. (Fall 2012). National Rosacea Society.
Last Updated June 14, 2022
Note: This page should not serve as a substitute for professional medical advice from a doctor or specialist. Please review our about page for more information.