Coloboma: What Is It, Causes & Treatment
Coloboma is an eye abnormality that people are born with. It can affect any part of the eye, lead to vision problems, and cause vision loss in extreme cases.
It is estimated that coloboma affects 1 in 10,000 people. This eye condition usually does not change a person’s eye appearance, and it does not affect vision. This is why it can be undiagnosed in some people.
How Does Coloboma Develop?
As babies develop during pregnancy, tissues grow on either side of the optic fissure. The tissue will connect at some point into a formed whole. This is how the eye structure develops.
But when something interferes with the process, there will be a hole, which is coloboma. According to the American Academy of Ophthalmology, this eye condition is genetic, so it can pass from parents to their children.
What Are the Causes of Coloboma?
It is largely believed that coloboma is caused by a genetic disorder that affects a baby’s eye when they are still developing during pregnancy.
During the last two months before a baby is born, a seam known as the optic fissure closes to form the eye’s structure. However, when the fissure fails to close completely, it leads to coloboma in one or both eyes of the baby.
Another major cause of coloboma is related to genes. Some studies have shown links between particular genes in parents and the likelihood that their children will be born with coloboma. However, further research is still required to identify exactly which genes cause them.
Finally, certain environmental factors that affect early development can also increase the risk of coloboma, including drinking alcohol or smoking tobacco products while pregnant.
Symptoms of Coloboma
The symptoms of coloboma often vary depending on where in the eye it occurs.
This eye condition is usually detected in infancy by a doctor. But it is also common to detect it in adulthood.
Here are some of the major symptoms of coloboma:
- Light sensitivity
- Misalignment of the eyes
- Poor vision or vision loss
- A defect in the iris
Risk Factors
One of the most notable risks of coloboma is that it can lead to various eye diseases. A coloboma on the eyeball or inside the eyeball creates a weak spot. This vulnerability can result in changes in pressure or changes in optimal function. These changes may cause other eye health issues.
Coloboma increases the risk of the following:
Glaucoma
A coloboma can alter the way the eyes drain, leading to pressure buildup within an eye. The optic nerve is sensitive to pressure, and if it gets higher, it can cause vision loss.
Cataract
While age-related cataracts are common in seniors, people with coloboma are more likely to develop cataracts at a younger age.
Retinal Detachment
If the coloboma is on the optic disk or retina, it can deteriorate the integrity of an eye. In extreme cases, the tissues at the back of the eye may pool out.
Treatment for Coloboma
While there is no direct treatment to cure coloboma, there are corrective measures available depending on which part of the eye is affected, the severity of the effect, and whether or not there are other defects.
Here are various treatments for specific types of coloboma:
Iris Coloboma
For this type of coloboma, a special contact lens is fitted on the eyes to cover the keyhole-shaped pupil to make it look round. This can enhance the cosmetic appearance of the eye and reduce light sensitivity.
Surgery may also be ideal for some people, where the gap in the iris is stitched together to reduce light sensitivity and correct the pupil shape.
Eyelid Coloboma
This type of coloboma requires surgery to protect the cornea and for cosmetic reasons. However, if the coloboma is small, the cornea will be protected with ocular lubricants. Then, immediate surgery will be performed to close the defect as it ages.
Retinal Coloboma
This type of coloboma also requires surgery, especially in the case of retinal detachment.
Complications of Coloboma
Colobomas can cause some complications. For instance, an eyelid coloboma can leave part of the cornea exposed, leading to extreme dryness because of the evaporation of the tears.
In addition, in cases of optic disc and retina colobomas, unusual blood vessels may grow right near the coloboma and trigger bleeding, which in rare cases, may lead to loss of eyesight.
Living With Coloboma
Many people who have colobomas can live their lives fully without any complications. However, some people may have vision difficulties because of the unique structure of the eye and may have to make a few lifestyle changes.
The presence of coloboma can make it difficult to focus the eyes. The impact of coloboma varies depending on the size of the gap and the part of the eye one uses.
For instance, if the gap is too small, one might only need glasses to read. Subsequently, some people may see things right in front but find it hard to see things on the side. While corrective lenses like glasses or contacts won’t fully correct vision, they can help.
It is important for people living with coloboma to have regular eye exams throughout childhood and adulthood. These exams will monitor eyesight and ensure that any other problem is properly managed.
Coloboma FAQs
What causes coloboma?
Coloboma occurs when the eye of the baby does not develop normally during gestation due to abnormal genes that affect eye development. It can run in a family.
In addition, environmental factors, such as drinking alcohol or smoking tobacco products during pregnancy, can increase the risk for coloboma.
What does a person with coloboma see?
Certain types of coloboma, such as retinal colobomas and those affecting the optic nerve, can affect vision. The vision loss that occurs cannot fully be corrected with glasses.
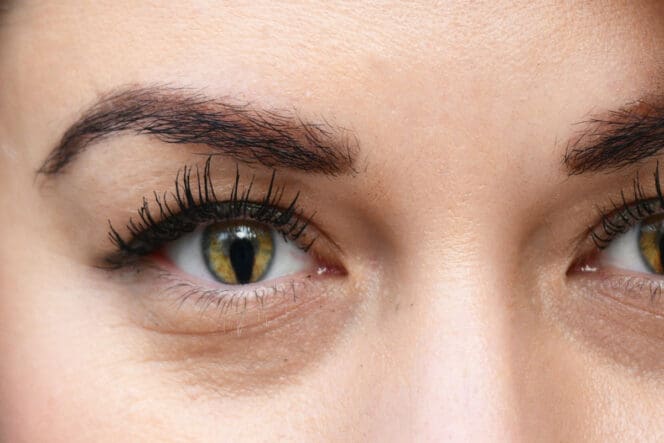
Colobomas mostly affect the iris, the tissue that gives the eye color. If the coloboma is partial, the pupil may look oval, but if a large part of the lower iris is missing, the pupil will look like a keyhole shape. Generally, people with iris coloboma have fairly good vision.
Can coloboma be cured?
No, there is no cure for coloboma. There are various treatments, such as surgery or colored contact lenses to improve the aesthetic appearance of a coloboma.
If low vision is a result of coloboma, treatment approaches include corrective lenses like glasses and low-vision aids. It might be necessary to wear an eyepatch to prevent amblyopia (lazy eye).
Babies and children with coloboma should be under the care of a pediatric optometrist or ophthalmologist as they are at higher risk for other eye conditions.
How common is coloboma?
About 1 in every 10,000 babies is affected by coloboma.
References
-
What Is a Coloboma? (January 2022). American Academy of Ophthalmology.
-
Ocular Coloboma—A Comprehensive Review for the Clinician. (March 2021). Eye.
-
ABCB6 Mutations Cause Ocular Coloboma. (January 2012). American Journal of Human Genetics.
-
Identification of 4 Novel Human Ocular Coloboma Genes ANK3, BMPR1B, PDGFRA, and CDH4 Through Evolutionary Conserved Vertebrate Gene Analysis. (May 2022). Genetics in Medicine.
-
Review of Evidence for Environmental Causes of Uveal Coloboma. (July–August 2022). Survey of Ophthalmology.
-
An Update on the Genetics of Ocular Coloboma. (May 2019). Human Genetics.
-
Coloboma. Royal National Institute of Blind People
-
What Is a Coloboma? (November 2020). American Association for Pediatric Ophthalmology and Strabismus.
-
Coloboma. National Eye Institute.
-
Who Is at Risk for a Coloboma? (April 2018). American Academy of Ophthalmology.
-
Cataract Surgery in Eyes With Associated Coloboma: Predictors of Outcome and Safety of Different Surgical Techniques. (March 2016). Indian Journal of Ophthalmology.
-
Coloboma Associated Retinal Detachment: Characteristics, Surgical Management, and Outcomes. (April 2014). Investigative Ophthalmology & Visual Science.
-
Risk of Retinal Detachment in Children With Ocular Coloboma. (January 2022). Ophthalmology.
-
Iris Coloboma Managed With a Prosthetic Contact Lens: A Case Report and Review. (April 2009). Clinical and Experimental Optometry.
-
Surgical Outcome of 21 Patients With Congenital Upper Eyelid Coloboma. (March 2010). International Journal of Ophthalmology.
-
Colobomas and Amblyopia. (November 2011). JAMA Ophthalmology.
-
Incidence, Ocular Findings and Systemic Associations of Ocular Coloboma: A Population-Based Study. (January 2012). JAMA Ophthalmology.
Last Updated August 9, 2022
Note: This page should not serve as a substitute for professional medical advice from a doctor or specialist. Please review our about page for more information.