Home / Eye Surgery /
Trabeculectomy Surgery: Uses, Risks, the Procedure & and More
Trabeculectomy is one of the most common glaucoma surgeries that creates a pathway for fluid to drain from the eye. Typically, it is used to reduce eye pressure and prevent glaucoma from getting worse.
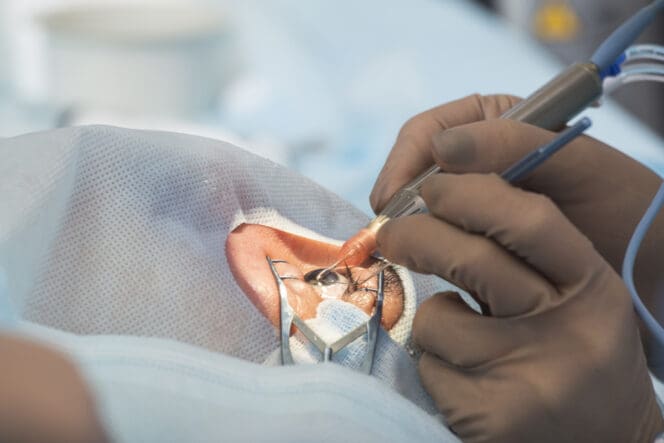
What Does Trabeculectomy Treat?
Trabeculectomy is designed to stop the progression of glaucoma. The surgery creates a pathway that enables fluid to drain from the eye.
Trabeculectomy surgery doesn’t restore vision. However, it does prevent future vision loss and can prevent glaucoma from getting worse.
Glaucoma is a disease where high eye pressure damages the optic nerve, resulting in loss of vision. Without treatment, patients lose peripheral vision and eventually central vision. Ultimately, if not treated, glaucoma can result in complete blindness.
Glaucoma is the leading cause of blindness in the United States, affecting 3 million people. Early detection and treatment are the most important ways to prevent loss of vision from glaucoma.
Benefits of Trabeculectomy
Numerous studies confirm that trabeculectomy is highly effective in treating advanced glaucoma.
Typically, glaucoma medicines and laser treatments are the first line of defense in glaucoma. However, if these have not helped your condition, it’s reassuring to know that glaucoma surgery can provide relief from excess pressure.
If a previous trabeculectomy has not worked successfully, secondary surgery may be effective. To intensify the second procedure, additional therapies may be used to reduce inflammation as well as scarring.
How to Prepare for Surgery
Your doctor may have specific recommendations as you prepare for surgery. You may need to stop taking some medications, such as blood thinners, before the operation. Avoid eating after midnight the day of the procedure.
Arrange to have someone drive you to and from the surgery. Additionally, check your schedule following surgery so you can avoid lifting heavy objects or exerting yourself for several weeks.
The Procedure
Trabeculectomy is designed to treat open-angle glaucoma, which is the most common type of glaucoma in the United States.
Typically, trabeculectomy is performed in a hospital operating suite. The entire procedure often takes under an hour.
Before the surgery, you will get IV medications to aid relaxation. Most patients are awake but relaxed and pain-free due to the calming medication. Expect your care team to numb the eye, so you will not feel pain during the surgery.
Your surgeon will make a tiny incision in the top of your eye, in the white of your eye, underneath the eyelid. A flap is cut creating an opening into the interior of the eye. Another opening may be created at the edge of the iris to prevent iris tissue from blocking the flow of fluid.
The incision will not be visible after the operation. The edges of the flap are reattached with sutures to help control the flow of fluid. The filmy skin covering the eye is also sutured around the flap.
After these procedures, it’s easier for excess fluid to leave the eye. When the fluid escapes, it creates a bubble, also called a filtration bleb. This bubble is usually underneath the upper eyelid and not visible without lifting the lid.
This pocket allows extra fluid to drain out of the eye and get absorbed by the surrounding tissue. The result is a reduction in excess pressure.
Following the procedure, some patients may need a short office laser procedure to break sutures and allow the trabeculectomy to be more successful.
Talk with your physician to determine the best options for your condition.
Recovery From Trabeculectomy
Typically, patients have this procedure on an outpatient basis.
Expect to have some soreness after the surgery. Most often, your doctor can recommend a pain medication that can be purchased over the counter.
Common Symptoms During Recovery
It is common for vision to be temporarily blurry in the days following surgery. You may experience redness, irritation, swelling, and feeling as if there is something in the eye.
Your doctor will prescribe eye drops to reduce symptoms and prevent infection. Expect to use these drops for several weeks after the surgery.
In the days and weeks following the procedure, vision will improve. Haziness will continue to clear each day.
Best Practices for Recovery
Use common sense and attention to hygiene to care for your eye during recovery:
- Use steroid eye drops as prescribed to encourage healing and help prevent scar tissue from forming.
- Use eye shields to protect your eye while you sleep.
- Resist rubbing your eyes.
- Avoid lifting heavy objects or straining yourself.
- Do not swim.
- Avoid using eye cosmetics such as eye creams and makeup.
- Do not wear contact lenses until advised to by your surgeon.
Watch out for any unusual or rare problems, such as bleeding, thick discharge, swelling, eye pain, or diminished vision. Call your doctor if you have concerns or experience problems during recovery.
Full recovery from trabeculectomy can take up to 12 weeks. Most people can return to work after about two weeks.
Expect frequent visits with your doctor during the first two months after surgery. These checkups may be one to two times per week, as your doctor monitors the healing process.
You’ll usually need to continue applying steroid and antibiotic eye drops for about three months.
Trabeculectomy Success Rates
According to the National Eye Institute, trabeculectomy surgery has a high success rate. It lowers eye pressure in 7 out of 10 people.
Risks & Complications
Risks of trabeculectomy vary depending on the anatomy of your eye, your age, and specific health conditions. These are the most common risks:
- Eye pressure remains high: Scarring around the surgical area can cause eye pressure to remain high. If this occurs, the scar tissue may be broken up, or a new surgery may be needed to reduce eye pressure.
- Leakage: Sometimes, there is fluid leakage from the site of the surgery. This may heal on its own or require another surgery.
- Eye pressure is too low: If the surgery drains too much fluid, eye pressure can drop below optimal levels. This may be only a temporary condition, or it may require another surgery to adjust the levels.
- Bleeding in the eye: This is a rare risk, but bleeding can occasionally occur inside the eye. This could cause vision loss if left untreated.
- Infections: Eye surgery has the potential for infections. These can be monitored and treated swiftly.
- Cataracts: Trabeculectomy surgery can increase the rate of cataract formations. Cataract surgery is typically highly successful in correcting the problem.
Alternative Surgical Options
Trabeculectomy is just one of the surgical options available for glaucoma. The alternative options are MIGS, laser treatments, stents, and surgery.
- MIGS: This is a new approach, called minimally invasive glaucoma surgery (MIGS). This method lowers eye pressure and has a faster recovery period. According to the American Academy of Ophthalmology, this treatment is used for mild glaucoma and offers relief with fewer side effects or risks.
- Lasers: These can be used to slow down the rate of fluid production. Office-based laser therapy and eye drops are often successful in helping glaucoma patients lower eye pressure.
- Glaucoma implant surgery: This is an alternate procedure used for specific types of glaucoma. This procedure uses a tiny tube called a shunt to drain excess fluid from the eye. Stents or shunts make a pathway to drain fluid.
These stents may be placed inside or outside the eye. It’s a hospital procedure that usually takes one to two hours.
- Tissue removal: Another surgical option is to remove tissue inside the eye to increase natural drainage.
Talk with your physician to evaluate the best surgical options for your situation.
References
-
Glaucoma: Trabeculectomy. (October 2015). American Academy of Ophthalmology.
-
Trabeculectomy. John Hopkins Medicine.
-
Glaucoma Surgery Recovery: What You Need to Know. John Hopkins Medicine.
-
Glaucoma. John Hopkins Medicine.
-
Glaucoma Surgery. National Eye Institute (NEI).
-
Trabeculectomy Surgery for Glaucoma. WillsEye Hospital.
-
MIGS: Expanding Options for Glaucoma Treatment. (February 2018). EyeNet Magazine. American Academy of Ophthalmology (AAO).
-
Glaucoma. National Eye Institute (NEI).
Last Updated May 4, 2022
Note: This page should not serve as a substitute for professional medical advice from a doctor or specialist. Please review our about page for more information.