Home / Eye Surgery /
Scleral Buckle Eye Surgery Explained
Scleral buckle eye surgery is one option for reattaching a retina. It is often combined with other surgical techniques as part of a more robust treatment plan.
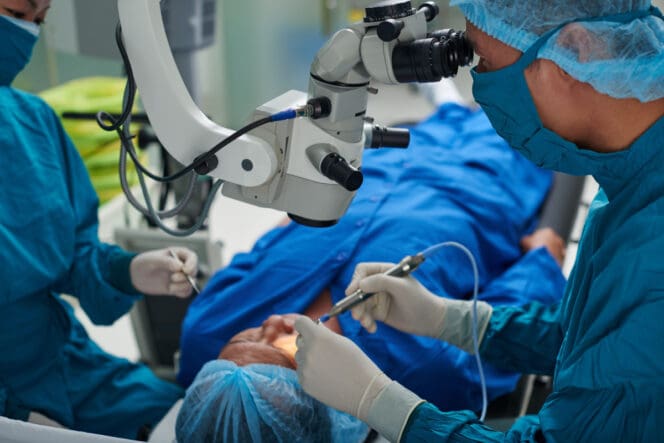
Scleral buckle eye surgery gets its name from a small band that is placed around the eye (the buckle), which helps keep everything in place after the surgery.
The Goal of Scleral Buckle Eye Surgery
A scleral buckle procedure is a form of retinal detachment (RD) repair. While less invasive methods are preferable when treating retinal detachment, severe cases require more involved methods (namely scleral buckling or vitrectomy) to fix.
There is no chance of a retinal detachment getting better without medical intervention. A repair of some kind is necessary to avoid permanent vision loss.
Candidates for Scleral Buckle Eye Surgery
Candidates for this surgery include people who have a severe case of retinal detachment and for whom less invasive alternatives will not work. The signs you may have had a retinal detachment include the following:
- Floaters
- Unexplained light flashes
- The appearance of a “curtain” in your vision
If you experience any of the above symptoms, treat them as an emergency. Retinal detachment is a serious condition that can often lead to permanent vision loss. Even if your doctor decides you don’t need scleral buckle eye surgery, you still need treatment right away.
Signs That Surgery May Help
The three primary surgical options when dealing with rhegmatogenous retinal detachment are scleral buckling, vitrectomy, and pneumatic retinopexy (PR). Often, a combination of two or three of these options works best.
A rhegmatogenous retinal detachment is characterized by a small tear or break in the retina. It is the most common type of retinal detachment, usually caused by aging combined with other risk factors, such as extreme nearsightedness or eye injury.
A medical professional will determine the specific type of RD you have developed. If you experience any signs of retinal detachment, you need medical intervention. Your doctor can determine if scleral buckling is a good choice for you.
How to Prepare for Scleral Buckle Eye Surgery
Your surgeon will have specific recommendations to prepare for surgery. Common preparations include the following:
- Stop certain medications that may interfere with the procedure or interact with necessary parts of your treatment.
- Do not eat or drink for 8 to 12 hours before your surgery beyond small sips of water to take any necessary medications.
- You’ll likely have eye dilation and an eye ultrasound prior to surgery.
The Scleral Buckle Procedure
While the experience may make you somewhat anxious, scleral buckling shouldn’t be painful. Many times, you will be given medication that causes you to sleep. If not, anesthesia will be used so you don’t feel pain, and you will be given medication to stay relaxed.
During a scleral buckling procedure, the eye is dilated and then exposed with special tools to keep it in position. A precise incision is made into the eye. Through that incision, a surgeon uses an ophthalmoscope. This is a special tool they can use to view the patient’s retina.
The doctor then uses a tool to freeze your retina to the inner wall of the eye, although sometimes a different method is used to achieve the same result. A buckle is put around the outside of the eye. This is where the surgery gets its name. This buckle keeps the retina in place and is often permanent.
Your doctor may decide that they need to drain some fluid from under your retina. This is normal but doesn’t always happen.
Recovery Timeline & Post-Op Care
After your surgery, antibiotic ointment may be applied to the eye, and you will get an eyepatch to wear during your recovery. You may be prescribed antibiotic or anti-inflammatory eye drops, usually for one week. This helps your eye heal and prevents infection and other complications.
Because this surgery involves anesthesia and putting a patch over one eye, you will need someone to drive you home. Barring complications, most patients return to normal activities within a couple weeks.
Your eye may hurt as you recover, although severe pain isn’t normal. The patch usually isn’t worn for more than a day or two.
If your vision seems worse or you experience any unexplained or severe symptoms, contact your doctor right away. You also will have a follow-up appointment scheduled after your surgery, and your doctor will then make sure you are recovering as expected.
Risks of Scleral Buckle Eye Surgery
Infection and swelling are common risks with almost any eye surgery, both of which can cause permanent damage if left untreated.
Sometimes retinal detachment surgery doesn’t manage to fully reattach the retina, and further surgery is required. Surgery can sometimes increase pressure in the eye, which can potentially cause glaucoma and permanent vision loss if not addressed.
An estimated 1 in 10 retinal detachments cannot be repaired, in which case permanent vision loss occurs.
Expected Outcomes of Scleral Buckle Surgery
The prognosis for retinal repair is good, with about 9 in 10 detachments successfully repaired. In many cases, a patient’s vision returns to the same level it was before the surgery.
Generally, the primary determining factor in the quality of vision for retinal repair in a successful surgery is the macula’s involvement. If the macula wasn’t involved, vision returns to normal. If it was involved for less than a week, vision returns but not to normal levels. The longer the macula was detached, the less positive the result usually is.
References
-
Retinal Detachment Repair. (August 2020). MedlinePlus.
-
Retinal Detachment. MedlinePlus.
-
Scleral Buckling. (2022). University of Rochester Medical Center.
-
Scleral Buckling for Rhegmatogenous Retinal Detachment. (December 2021). American Academy of Ophthalmology.
-
Types and Causes of Retinal Detachment. (December 2020). National Eye Institute.
-
Evaluation and Management of Suspected Retinal Detachment. (April 2004). American Family Physician.
Last Updated May 23, 2022
Note: This page should not serve as a substitute for professional medical advice from a doctor or specialist. Please review our about page for more information.