Home / Eye Surgery /
Raindrop Eye Surgery: Everything You Need to Know
Raindrop surgery was a preferred surgical method of treating presbyopia. It had advantages over other similar procedures because it did not involve reshaping the cornea, but candidates had to be between 40 and 65 years old. The procedure was halted after the U.S. Food and Drug Administration issued a recall when a study showed 75 percent of people who opted for the procedure developed corneal haze.
What Is Raindrop Surgery?
Raindrop eye surgery was an innovative way to safely treat presbyopia without having the new, improved vision affected by further aging.
The procedure called for a raindrop-shaped inlay to be fitted underneath the cornea. The purpose was to treat presbyopia, an age-related refractive error that affects people who are 40 years old and older.
A cornea and lens that loses mass or change shape cause presbyopia, which triggers near-vision loss and makes it difficult to focus clearly and consistently when you need your eyes to re-focus from close-up objects to faraway objects, and vice versa.
The loss of close-up vision can be a challenge to live with because of how much near vision we use in day-to-day life: reading, texting, using the computer, etc.
How Does Raindrop Surgery Work?
The surgery got its name because of a raindrop inlay, a tiny, almost microscopic device that doctors implant just under the cornea. The implant changed the angle at which light refracts into the eye to create a clearer image on the retina. The device consisted of 80 percent water and resembles a small contact lens.
When implanted, the raindrop inlay increased the steepness of the center of the eye, correcting the refractive error caused by the loss of mass.
Who Is a Candidate?
The goal of raindrop surgery was to improve near vision for the non-dominant eye. But not everyone could have the procedure. To be a candidate, you must match the following criteria:
- You are in the age range of 41 to 65 years
- You have presbyopia without suffering other refractive errors
- You cannot focus on near objects or small print text
- You require glasses with a magnifying power from +1.5 to +2.5 dioptres of power to read
- You have no underlying conditions like glaucoma or cataracts
- You have not had other eye surgeries in the past
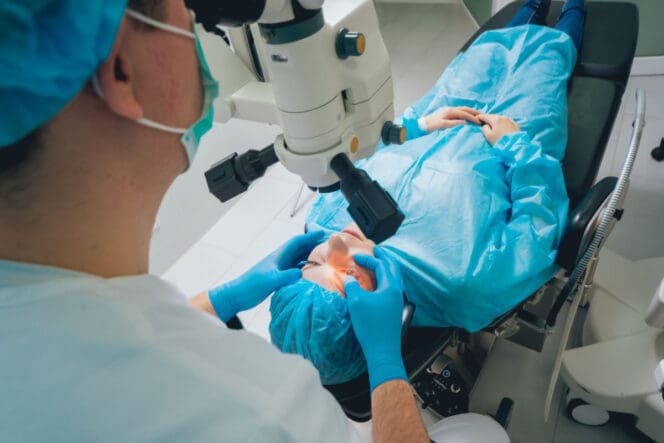
Raindrop vs. Other Eye Surgeries
Prior to Raindrop surgery, doctors turned to other surgeries to treat presbyopia, including LASIK and other laser procedures. Another option was using conductive keratoplasty to reshape the cornea using either a heat probe or radio waves.
The problem with these alternatives is that because the refractive error is age-related, the surgical effects wear off with time, necessitating further surgery. In the case of procedures like LASIK, it may not be possible to conduct another surgery if your cornea is extra thin.
The results of Raindrop surgery were not affected by increased aging because the procedure does not alter or replace your natural lens or cornea.
Benefits
The Raindrop eye surgery had several advantages over other procedures in treating presbyopia, including:
- It did not remove any tissues from the cornea.
- It was not painful.
- The surgery was safe and fast.
- It offered a speedy recovery, and people gained improvement in their near vision ability the next day.
- Over time, the improved near vision did not continue to deteriorate with advanced aging like other methods.
The Procedure
The procedure starts with a complete eye exam to understand the refractive era, gauge your overall eye health, your corneal health and your suitability for the procedure.
Two days prior to the procedure, the doctor will instruct you to use steroid eye drops. On the day of the procedure, the doctor will give you anesthetic drops to numb your eyes. The doctor then holds your eyelids open with a device to prevent you from blinking.
Using a laser, he will cut open a flap on the cornea and then implant the Raindrop inlay in one of the corneal layers. He then replaces the flap back in place and confirms the positioning of the inlay using a microscope.
The incision and the flap are then smoothed over, there is no need for stitches, and the procedure is complete in about 10 minutes.
Recovery
Patients tend to resume normal activities within a day or two after surgery though the time varies. You will also need to use an eye shield when you sleep for protection for about four weeks.
The doctor will also give you medication to prevent inflammation and other potential side effects after the surgery. The doctor will advise you on the best care, including activities to avoid and the schedule for a follow-up examination.
Risks
Raindrop eye surgery carries several risks, including:
- Worsening of glares, halos and blurred vision
- Chronic eye dryness
- Increased risk of cataracts forming
- Increased eye pressure
- Requirement for additional surgery
Complications include:
- Corneal haze
- Issues at the back of the eye
- Inflammation
- Scarring
- Melting corneal tissue
Costs
One of the challenges of Raindrop eye surgery is its cost, which typically ranges between $4,000 and $5,000. Despite the seriousness of presbyopia, most vision-related insurers consider Raindrop surgery to be cosmetic and will not cover any costs.
Success Rates and Outlook
In a clinical trial to test the effectiveness and safety of the procedure, 92 percent of people in the study recorded better near vision eyesight. But in 2019, the FDA issued a recall of the inlay after a post-approval study showed it increased the risk of corneal haze.
Some 75 percent of people in that study had corneal haze. The procedure is currently not available for new patients, and the company that innovated it is no longer in business. It, however, inspired other corneal inlays, several of which are based on it, are still in the market, and are available. These include the Flexivue microlens and KAMRA implants.
References
-
FDA Recalls Raindrop Inlay (March 2019). Review of Optometry.
-
Raindrop Surgery Cost (August 2018). Howmuchisit.org
-
What Is Presbyopia? (September 2017). American Academy of Ophthalmology (AAO).
-
FDA Approves Implantable Device That Changes the Shape Of The Cornea To Correct Near Vision (June 2016). US Food and Drug Administration.
-
Raindrop Near Vision Inlay: Patent Information Brochure. U.S. Food and Drug Administration (FDA).
Last Updated June 8, 2022
Note: This page should not serve as a substitute for professional medical advice from a doctor or specialist. Please review our about page for more information.