Home / Eye Surgery /
Laser Iridotomy Eye Surgery: Procedure, Side Effects, and More
Ophthalmologists perform laser iridotomy to alleviate eye pressure that threatens to cause long-term vision loss. The surgery takes only a few minutes, and its purpose is to minimize the development of glaucoma, the second-leading cause of blindness. The outpatient procedure can halt further vision loss, but it cannot reverse vision loss that has already occurred.
What Is Laser Iridotomy Eye Surgery?
Laser iridotomy is the surgical treatment of abnormally high eye pressure. It is a medical precaution that your ophthalmologist (eye surgeon) may recommend if you have angle-closure glaucoma or narrow angles that are risk factors for glaucoma.
Narrow angle is when your iris is abnormally close to the cornea. With little, if any, fluid draining from your eye, pressure can quickly increase inside and damage the optic nerve.
Optic nerve damage that occurs this way is called angle-closure glaucoma, and it can slowly cause permanent vision loss. People on schedule for phakic lens implantation surgery may also need a laser iridotomy to prevent glaucoma.
How Does a Laser Iridotomy Work?
Laser iridotomy creates a tiny opening in the iris, providing an alternative channel for excess fluid (aqueous humor) to flow out of the eye smoothly. Once normal fluid drainage is reestablished, pressure on the optic nerve often decreases to a healthy range.
Who Is a Candidate?
Roughly 3 million people in the United States have glaucoma, the world’s second-leading cause of blindness. Eye doctors recommend laser iridotomy once careful assessment shows that the procedure can safely prevent vision loss in a patient with narrow angle glaucoma.
You may be eligible for the surgical puncturing of your iris if:
- You have the angle closed for 50 percent or more of the available drainage channel, causing abnormal eye pressure or optic nerve damage
- You’re at risk of abnormal eye pressure buildup and optic nerve damage due to a closed angle
Cooperative Patients
The cause of the angle closure also determines whether a patient is eligible for a laser iridotomy. If the problem is medication-induced, puncturing the iris may not offer any benefit.
Benefits
Laser iridotomy is a potential vision saver for millions of people living with or at risk of angle-closure glaucoma. Among the benefits of the procedure include:
- Glaucoma treatment: If you have chronic angle closure glaucoma, having laser iridotomy can help relieve excess eye pressure, preventing any further optic nerve damage. This intervention often results in a widening of the angle and can prevent blindness in the affected eye.
- Glaucoma prevention: Your vision may be safe if you have a closed angle that has not pushed your eye pressure to an abnormally high range or caused optic nerve damage. A recent study showed that having a laser iridotomy can lower the risk of angle-closure glaucoma further in patients like you.
- Phakic lens implantation: Your doctor may recommend a laser iridotomy ahead of a scheduled lens implantation surgery. This would prevent fluid and pressure buildup at the back of your eye after the procedure.
While timely laser iridotomy can prevent optic nerve damage due to narrow angles, it cannot reverse any vision loss that already occurred.
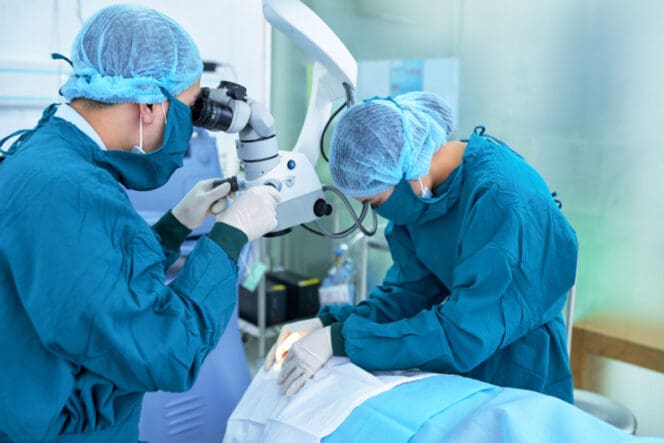
The Procedure
Laser iridotomy surgery usually takes place at the doctor’s and lasts only a few minutes. You will go home the same day.
Here’s how your eye doctor may perform the outpatient procedure:
- About 30 minutes before surgery, the surgeon will treat your eye with special drops that reduce the pupil’s size
- Numbing drops are placed in your eye to make the procedure as comfortable as possible
- The doctor places a large lens on your eye to help focus the laser
- The surgeon directs the laser on the outer edge (periphery) of your iris, slightly puncturing it
- Your doctor would normally check your eye pressure within an hour or so after the laser iridotomy surgery.
Recovery
Because laser iridotomy is minimally invasive, it allows you to resume your daily routine quickly, including driving home after the procedure. If all goes well, your optic nerve pressure should go back to healthy levels within minutes once an escape for the accumulated eye fluid has been created.
Most vision issues that remain after the surgery are temporary, such as blurriness and halos surrounding lights. For the majority of people who undergo the procedure, these effects resolve within six months. Your doctor will monitor your progress closely.
Puncturing any part of your eye can cause inflammation and swelling. You may need to use anti-inflammatory eye drops as instructed by your doctor for a few days to control any swelling of your iris.
Risks
These complications may occur in some patients after having a laser iridotomy:
- High eye pressure
- The laser may injure your cornea or lens, causing cloudy vision
- The opened channel may close in the future
- Vision problems like flashes or double vision
- Bleeding at the site of puncture, such as if new blood vessels in the iris caused the angle closure (neovascularization of the iris)
Costs
Laser iridotomy is not as expensive as other glaucoma-related eye surgeries. It is one of the least-invasive options, and neither involves operating room costs nor general anesthesia fees.
For the procedure, you may pay between $1,000 and $2,000 without insurance. The ability of laser iridotomy to prevent vision loss or halt the progression of chronic angle-closure glaucoma makes it medically necessary for many at-risk patients.
This medical necessity means that most health insurance carriers provide coverage for the vision-saving surgery. If you have a vision plan, review the fine print for any applicable limits, deductibles, or co-pays as these can impact your out-of-pocket costs for this treatment.
Success Rates/Outlook
In about 65 to 76 percent of people who undergo a laser iridotomy, the angle is opened. The primary goal is to reduce pressure on the optic nerve, so when this is achieved, the eye surgery is considered successful.
Approximately 1 in every 4 people who have the procedure do not receive the treatment benefit immediately, and some people may require another laser procedure or surgery to open the angle.
Also, because of age-related eye problems, such as cataract formation, the angle may close after initially opening with laser surgery. In that case, you may need the cataract surgically removed to reestablish drainage of fluid from your eye.
Ongoing Treatment
If you were using glaucoma eye drops before surgery, you likely will continue needing your medication even after successful angle opening surgery.
Studies show that some patients are at a high risk of developing a traumatic cataract one to six years after having a laser iridotomy. Eye pressure can also increase months after surgery.
To closely monitor any pre-operative complications, your ophthalmologist or optometrist may recommend long-term follow-up and management. Some people must use eye pressure medication for the rest of their life following iridotomy surgery.
FAQs
How long does it take to recover from laser iridotomy?
Minor complications of laser iridotomy, such as inflammation, usually resolve within a few days after surgery with proper medication. In rare cases, the procedure destabilizes vision, causing halos, blurred images and other visual side effects. These, too, are short-term and normally go away within six months.
What is the success rate of laser iridotomy?
Laser iridotomy works in 65 to 76 percent of people who have the surgery (opens the angle and eases eye pressure).
Is laser iridotomy painful?
Your surgeon will administer drops to numb your eye, which will reduce any discomfort during surgery. But some people might experience some mild pain.
References
-
Laser Iridotomy: Frequently Asked Questions. (March 16, 2022). Glaucoma Research Foundation.
-
Glaucoma Surgery: Types, Costs & Success Rates. (November 5, 2021). Nvision Eye Centers.
-
Laser Peripheral Iridotomy. (November 2, 2021). American Academy of Ophthalmology.
-
Laser Peripheral Iridotomy. (September 16, 2021). Hull University Teaching Hospital.
-
Don’t Let Glaucoma Steal Your Sight! (November 24, 2020). Centers for Disease Control and Prevention.
-
Lasers in Glaucoma. (November 2018). Indian Journal of Ophthalmology.
-
Phakic Intraocular Lenses (Before, During, & After Surgery). (January 8, 2018). The U.S. Food & Drug Administration.
-
Breaking Down Barriers: Iridotomy in Optometric Practice. (May 15, 2016). Review of Optometry.
-
Prognostic Factors for the Success of Laser Iridotomy for Acute Primary Angle Closure Glaucoma. (December 2009). Korean Journal of Ophthalmology.
Last Updated June 8, 2022
Note: This page should not serve as a substitute for professional medical advice from a doctor or specialist. Please review our about page for more information.