Episcleritis: Causes and Treatment
Women are more prone than men to develop episcleritis, especially women between the ages of 40 and 50. Many cases of the condition are mild, requiring no treatment or else artificial tears or corticosteroid drops. Redness and irritation are key symptoms, and there is usually little discomfort.
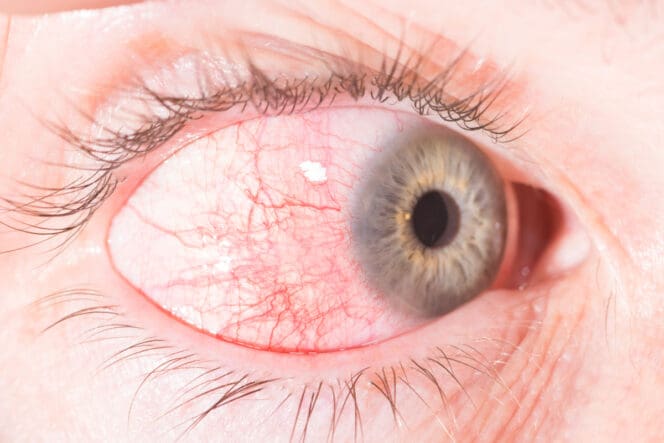
What Is Episcleritis?
Episcleritis refers to the unilateral (one eye) or bilateral (two eyes) inflammation of the episclera, the clear layer of the eye between the sclera, the firm white part of the eye, and the conjunctiva, a clear film that covers the eyeball.
Episcleritis is benign and self-limiting. That means it is usually harmless and clears on its own accord a few days after it begins. Although it may look like conjunctivitis, a more commonly witnessed eye infection, episcleritis doesn’t cause discharge.
The condition is slightly more common in women, especially those between the ages of 40 and 50, and it typically takes two to 21 days to clear out without medication or three to five days with medication.
Types
There are two types of episcleritis — diffuse and nodular. Of the two types, nodular episcleritis is more likely to occur because underlying systemic inflammation.
Both types cause mild discomfort and sensitivity to bright light. They also both make eyes feel tender when pressed.
Diffuse Episcleritis
Diffuse episcleritis represents about 70 percent of the diagnosed cases of the condition. It causes evenly bloodshot eyes and tends to be mildly discomforting. It sometimes causes the eye to redden all over or causes reddening in a small wedge shape at the corners of the eyes. This type of episcleritis can show up out of nowhere, but it also clears away much faster.
Nodular Episcleritis
Nodular episcleritis takes longer to take root but is also slower to heal. Aside from reddening the eyes, it causes small, inflamed nodules and bumps to appear in the episclera. About 30 percent of episcleritis cases are of the nodular type.
Causes
Episcleritis has no known direct cause. However, 26 to 36 percent of people who contract episcleritis are believed to have an underlying systemic disorder.
As a result, the condition is linked to a long list of diseases known to cause inflammation. They include, but are not limited to:
- Rheumatoid arthritis
- Crohn’s disease
- Psoriatic arthritis
- Reactive arthritis (Reiter’s syndrome)
- Ulcerative colitis
- Systemic lupus erythematosus
- Ankylosing spondylitis
- Relapsing polychondritis
- Pustulotic arthro-osteitis
- Cogan’s syndrome
- Behcet’s disease
- Dermatological diseases (rosacea, Sweet’s syndrome)
- Malignancies (Hodgkin’s lymphoma, T-cell leukemia)
- Foreign bodies in the eye
- Chemical injuries
- Infectious agents (spirochetes, myobacteria, bacteria)
- Protozoa (Toxoplasmosis, Acanthamoeba)
- Toxocara
- Medications (pamidronate, topiramate)
Episcleritis is most commonly associated with collagen-vascular diseases like rheumatoid arthritis. Numerous studies suggest that female adults are more at risk than male adults, but a study carried out on a pediatric population revealed that young males were affected more commonly than young females.
Children are rarely diagnosed with either type of the inflammation.
In addition to not having a specific cause, episcleritis does not have specific risk factors, either. The only link in people with eye disease is an associated systemic disease.
One study in particular showed that 51 percent of people with episcleritis suffered from a concurrent eye disease.
Signs & Symptoms
Episcleritis symptoms vary from mild to moderate depending on the type and severity of the condition. Symptoms include:
- Redness in one or both eyes (bloodshot eyes)
- Tearing (wateriness)
- Sensitivity to bright light
- Eye irritation, eye discomfort
- Slightly raised bumps covered in blood vessels (nodular)
- Prickly, hot or gritty sensation (nodular)
- Eye swelling
If you experience a deep, boring kind of pain and notice pink or purple eyeball coloration coupled with discharge coming from the affected eye, see a doctor immediately. Episcleritis rarely causes any eye discharge or photophobia (discomfort from bright light).
Episcleritis and scleritis share some symptoms, but episcleritis is less severe. Scleritis usually result in acute pain and sometimes a loss of vision.
Diagnosis
Eye doctors must deliver a thorough eye exam to diagnose episcleritis correctly. Your doctor or ophthalmologist conducts the exam to check:
- The color of your eyes
- The shade of the discoloration
These tests help professionals to determine whether you have episcleritis or scleritis. You may also be subjected to a kind of test known as a slit lamp exam.
This test entails the use of a microscope with a bright light (slit lamp) to observe the area in and around your eyes. The test ascertains whether there is increased eye pressure, which is a telltale indicator of problems such as glaucoma.
For this procedure, you may receive numbing eye drops first. The doctor uses a special contact lens, which they place directly onto your eyeball, to check the eyeball in order to establish an area of injection. This test also differentiates nodular episcleritis from scleritis.
If you experience recurrent cases of episcleritis but suffer from no known associated disease, the eye doctor may recommend systemic evaluation based on your medical history and examinations.
Treatment
Episcleritis does not always require treatment. The self-limiting condition gradually disappears within two to 21 days without medication.
But treatment can speed up the recovery process (and reduce discomfort). You have a choice among medical treatments, at-home treatments or a combination of the two.
Medical Treatment
For the mildest cases, using lubricating eye drops or ointment may be enough to alleviate the harsher symptoms. Some people find that using artificial tears containing tetrahydrozoline clears away the redness.
Tetrahydrozoline drops constricts blood vessels in the eye, which is how the medication helps with discoloration and redness.
If the discomfort is considerable, your eye doctor may recommend non-steroidal anti-inflammatory drugs (NSAIDs) to be administered orally or as eye drops.
Nodular episcleritis often requires supervised treatment from an ophthalmologist. Your eye doctor may administer corticosteroid eye drops that can speed up recovery significantly.
For the most part, however, episcleritis treatments address the underlying inflammatory conditions.
At-Home Treatment
Because episcleritis is mild, you can treat it at home by:
- Using a cold compress over closed eyes
- Using refrigerated artificial tear eye drops
- Protecting your eyes from strong outdoor light (sunglasses)
Episcleritis vs. Scleritis
Episcleritis and scleritis affect the episclera and the sclera, respectively. Here is a comparison table for the two conditions:
| Episcleritis | Scleritis |
| Mild, benign, and self-limiting | Severe and requires aggressive treatment |
| Causes irritation and mild discomfort | Causes mild to severe eye pain |
| Causes redness | Causes bluish or purple discoloration |
| Does not affect vision but may cause sensitivity to bright light | Causes blurred vision and sensitivity to bright light |
| Does not cause vision damage | Can cause permanent vision damage |
| Doesn’t harm other eye tissues | Can spread to deeper tissues of the eye |
Episcleritis shares multiple symptoms with scleritis, but its symptoms are much milder. Scleritis is more serious and can lead to long-term damage to the eye tissues.
Both conditions may have similar symptoms at the onset, but scleritis is usually far more painful and harder to manage without professional help.
Prevention
You cannot prevent getting a case of episcleritis. The best way to avoid the eye condition is to address its underlying cause, which is usually a systemic inflammatory disease such as rheumatoid arthritis.
Complications
Episcleritis usually does not develop complications, but in rare cases it can lead to scleritis. Scleritis may be accompanied by a host of other complications, including glaucoma, intraocular pressure, retinal detachment and glaucoma.
Someone with episcleritis is more likely to experience relapses, especially when the underlying cause is not addressed. The condition is also linked to anterior and intermediate uveitis, peripheral corneal infiltrates, and corneal dellen. In some cases, the steroidal medication one uses to manage episcleritis may cause glaucoma and cataracts.
References
-
Episcleritis. (August 2021). StatPearls.
-
Episcleritis and Scleritis. (August 2018). Patient.info
-
What is a Slit Lamp? (April 2018). American Academy of Ophthalmology
-
Is this a worrisome red eye? Episcleritis in the primary care setting. (February 2018). Journal of Community Hospital Internal Medicine Perspectives.
-
Diagnosis and treatment of episcleritis and scleritis. (September 2016). The Opthalmologist: Journal of the German Ophthalmological Society.
-
Clinical Characteristics of a Large Cohort of Patients with Scleritis and Episcleritis. (January 2012). Ophthalmology.
Last Updated May 16, 2022
Note: This page should not serve as a substitute for professional medical advice from a doctor or specialist. Please review our about page for more information.