Keratitis: Symptoms, Causes, and Treatment
Contact-lens wearers are at risk of developing keratitis, or corneal ulcers, an inflammation of the cornea.
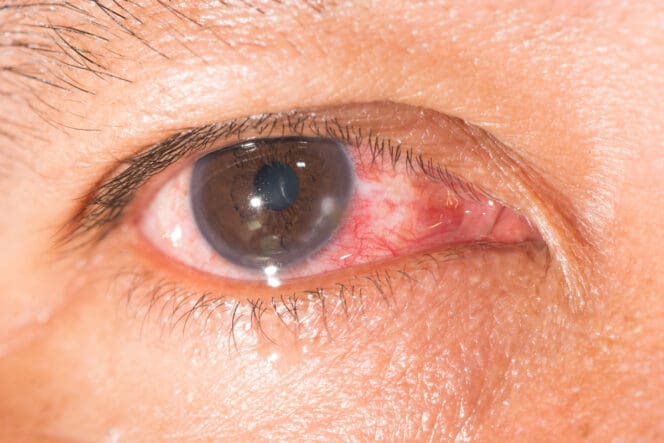
There are three types of keratitis, which can be bacterial or viral. Treatment — from ointments to medicated eyedrops —depends on the cause of the ulcers.
Humming
What Is Keratitis?
Keratitis is the irritation or inflammation of the cornea, your eye’s outermost part, which covers the iris and pupil. The condition is also known as corneal ulcer, and while it is treatable, it is the leading cause of corneal blindness.
Keratitis is a common condition, especially among those who wear contact lenses. If you suspect you might suffer from the disease, inform your eye specialist, as early detection is key to successful treatment.
Symptoms of Corneal Ulcers
Symptoms of keratitis include:
- Redness of the eyes
- Eye pain
- Blurred vision
- Watery eyes and excess tearing
- Deteriorating vision
- Light sensitivity
- Difficulty opening eyes
- Eye discharge
Types of Keratitis
Eye specialists put corneal ulcers into two major categories based on what causes them. These broad classifications are infectious and noninfectious keratitis.
Infectious Keratitis
Any of the following microorganisms can cause this form of keratitis:
- Fungi: Candida, Aspergillus, or Fusarium can all cause fungal keratitis, mainly affecting people who wear contact lenses. You can, however, also contract the fungal infection from outdoor spaces.
- Bacteria: The most common bacteria that can lead to keratitis are Staphylococcus aureus and Pseudomonas aeruginosa. Like in the case of fungal keratitis, you can get bacterial keratitis from improper use and care of your contact lenses.
- Viruses: Viral keratitis is most often the result of the infection with the herpes simplex virus. The disease develops and progresses from conjunctivitis to keratitis.
- Parasites: Acanthamoeba is a parasite that lives in various water bodies, including lakes and sometimes tap water. You can pick up the parasite when walking in wooded areas or swimming in natural water spaces. The infection from this parasite is known as Acanthamoeba keratitis.
Noninfectious Keratitis
Among the potential contributing factors and causes of noninfectious keratitis are:
- Weak immune system
- Wearing contact lenses for long without changing them
- Exposure to excess sunlight (photokeratitis)
- Eye injury from scratching
- Wearing your contact lenses when swimming
- Living in warm climates
- Allergies
How Is Keratitis Diagnosed?
An eye doctor’s first step in diagnosing corneal ulcers is reviewing your medical history and identifying any underlying symptoms. Doctors do not take the same diagnostic path for each case. There are so many root causes of keratitis that they must take varying approaches. For instance:
- In fungal and bacterial keratitis, doctors may have to scrape a small piece of your cornea for laboratory testing.
- A viral keratitis diagnosis does not require a lab test: the doctor needs only to review your medical history.
- Parasitic keratitis is tougher to diagnose. Doctors need to see the parasite causing the condition, often with the help of extensive lab testing.
During an examination, doctors may use a penlight or slit lamp. Penlights help them look closely at your eye and document any damage or changes.
In some cases, doctors may apply a stain to the surface of the eye to look at the extent of corneal ulters and surface changes.
Risk Factors Associated with Keratitis
Because keratitis is an inflammation of the eye, it can happen to anyone. However, some people stand a greater risk of developing the condition. Risk factors that make corneal ulcers more likely to develop include:
- Wearing contact lenses without accurately caring for them or cleaning them. Sleeping with your contacts can also increase the chances of developing keratitis.
- Someone who had a recent injury or infection of the eye is more at risk of developing the condition.
- People who have had the herpes simplex virus are also at risk.
- Someone with dry eyes is also prone to developing the condition, and so are people with complications in the eyelids and tear ducts.
How to Treat Keratitis
Treating corneal ulcers depends on what caused them. In the case of a scratched or injured cornea, you do not need any specific treatments, but doctors may prescribe an antibiotic ointment for comfort.
With viral keratitis, you’ll receive oral medication, eye drops or both. Antibiotics are the go-to therapy for bacterial keratitis. Artificial tears that lubricate the eyes, on the other hand, are the most common supporting therapy for all types of keratitis.
How Can You Prevent Keratitis?
Here are tips to reduce your risk factor and exposure levels to keratitis:
- Do not sleep with your contacts in.
- Change your contacts as advised by your eye specialist.
- Only use the recommended solution to clean your contacts.
- Wear protective eyeglasses when working with trees and plants.
- Include vitamin A in your diet.
- Wear sunglasses when exposed to bright sunlight.
Keratitis FAQs
Is keratitis contagious?
Yes, you can contract the condition by touching an infectious substance. Noninfectious keratitis is, however, not contagious.
What is the most common cause of keratitis?
Viral keratitis is the most common type of the disease, although there’s a significant number of people who get the condition from injury to the eye.
Can keratitis heal on its own?
Noninfectious keratitis can clear up on its own as your eyes heal. Infectious keratitis, however, needs timely medical intervention to avoid blindness or vision loss.
What is the difference between conjunctivitis and keratitis?
Conjunctivitis is the inflammation of the white part of the eye and the lines inside the eyelids. Keratitis is the inflammation of the clear covering of the eye. The former can be caused by many things, including viruses, while the latter can develop because of injury, parasites, fungi, bacteria, or viruses.
References
-
Herpes Simplex Keratitis. (November 2021). National Center for Biotechnology Information.
-
What is Conjunctivitis (Pink Eye). (November 2021). Centers for Disease Control and Prevention.
-
Acanthamoeba Keratitis. (August 2021). National Center for Biotechnology Information.
-
Healthy Contact Lens Wear and Care. (May 2021). Centers for Disease Control and Prevention.
-
Corneal Blindness: A Global Perspective. (May 2001). World Health Organization.
Last Updated April 29, 2022
Note: This page should not serve as a substitute for professional medical advice from a doctor or specialist. Please review our about page for more information.